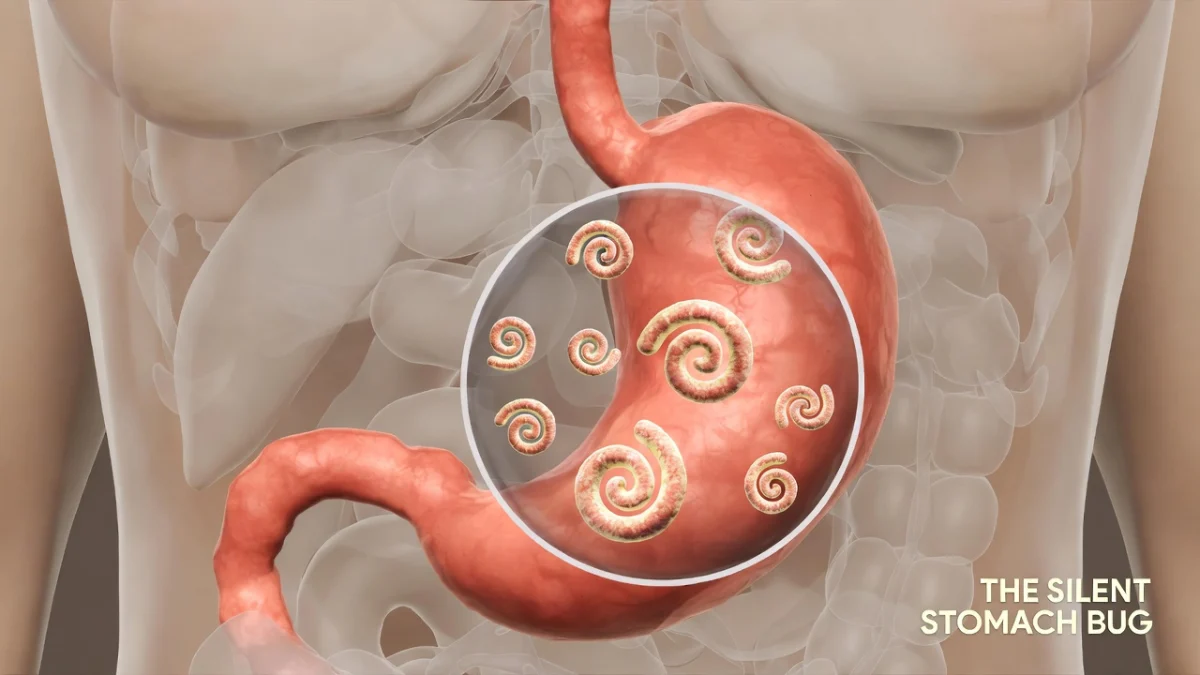
Most people have never heard of Helicobacter pylori, yet this little spiral-shaped bacterium quietly lives in the stomachs of billions worldwide. In Germany alone, roughly half of adults carry it, with rates climbing as high as 70–90% in folks over 65. For many, it causes zero trouble. But for others, it quietly sets the stage for painful ulcers, chronic stomach inflammation, and in rare cases, even raises the risk for stomach cancer down the line.
The good news? Once doctors spot it, treatment can wipe it out completely in most cases. The tricky part is knowing exactly who needs testing and what the smartest treatment path looks like in practice. Guidelines have evolved over the years, balancing effectiveness against rising antibiotic resistance and keeping things practical for everyday doctors and patients.
Also Read
In this post we’ll walk through the current thinking on when testing makes sense, the best ways to diagnose it, how treatment usually goes, and why follow-up matters – all based on established German recommendations that remain highly relevant as we move through 2026.
Why This Bacterium Matters More Than You Might Think
Helicobacter pylori (often shortened to H. pylori) is one of the most common chronic infections on the planet. Kids usually pick it up early in life, often within the family, and once it’s there it tends to stick around for decades unless treated. Adults rarely get newly infected.
In places like Germany, prevalence stays relatively low compared to many parts of the world – about 3% in children and around 48% overall in adults – but it still climbs steadily with age. That’s important because the longer it lingers, the higher the chance it can damage the stomach lining.
The main issues it causes include:
- Peptic ulcers in the stomach or duodenum (very common link)
- Chronic inflammation of the stomach (gastritis)
- Functional dyspepsia (ongoing upper belly discomfort without obvious cause)
- Increased bleeding risk when combined with painkillers like aspirin or NSAIDs
- A small but real contribution to stomach cancer and certain lymphomas in susceptible people
Eradicating the bug heals most ulcers, cuts bleeding risks dramatically in at-risk patients, and can ease symptoms for a lucky subset of those with indigestion.
Who Really Needs Testing? Clear Indications Matter
Unlike some countries that push broad “test-and-treat” for everyone with stomach complaints, Germany takes a more targeted approach. Testing only happens when there’s a solid reason to treat if positive – no fishing expeditions.
Strong reasons to test and eradicate include:
- Active or past peptic ulcer disease
- Planning long-term use of NSAIDs or low-dose aspirin if there’s any ulcer history
- Bleeding in the stomach/duodenum while on those painkillers
- Certain rare conditions like gastric MALT lymphoma
Weaker but still reasonable reasons (“can” consider) include unexplained indigestion, where treatment helps about 1 in 10 people long-term.
Routine screening? Not recommended here due to the lower prevalence and good access to endoscopy. Testing without a plan to treat is pointless.
Special note for everyday scenarios: If someone starts regular aspirin or ibuprofen and has ever had an ulcer, check for H. pylori first. Eradicating it before starting can halve the bleeding risk.
How Doctors Actually Diagnose It
Diagnosis relies on reliable tests that detect active infection. Two main categories exist: invasive (during endoscopy) and non-invasive.
Common reliable options:
- Urea breath test (you drink a solution and breathe into a bag – very accurate)
- Stool antigen test (simple sample from home)
- Rapid urease test or histology from stomach biopsies (during scope)
- Culture from biopsies (mainly for checking antibiotic resistance)
A couple of rules apply: usually need two positive tests to confirm, except in clear ulcer cases where one often suffices. Antibody blood tests? Not useful for active infection – they stay positive even after successful treatment.
Things that mess up results: recent antibiotics, strong acid blockers (PPIs), or active bleeding can cause false negatives. Doctors usually stop PPIs for a couple of weeks before testing.
In kids, guidelines push for biopsies early to guide resistance-based treatment.
Treatment – What Works Best in Practice
The goal is complete eradication. Success rates need to hit at least 80–90% to be worthwhile, but resistance makes it harder than it used to be.
In Germany, the standard approach still starts with classical triple therapy: a proton pump inhibitor (PPI like omeprazole) plus clarithromycin and amoxicillin (or metronidazole) for 7–14 days. It’s simple and works well when resistance is low.
But clarithromycin resistance is the big enemy – higher in southern/eastern Europe or after prior macrolide use. If risk looks elevated, doctors switch to bismuth quadruple therapy as an alternative (PPI + bismuth + two antibiotics, usually tetracycline and metronidazole).
Key practical tips for better outcomes:
- Pick the regimen based on local/personal resistance clues
- Explain everything clearly – people who understand stick to it better
- Use adequate PPI doses and timing
- Treat for the full course even if symptoms vanish early
For kids, treatment often follows resistance testing from the start.
After treatment, confirm success – it’s strongly recommended regardless of why you treated.
Confirming It’s Really Gone – Don’t Skip This Step
Wait at least four weeks after finishing antibiotics (or two weeks off PPIs) before checking.
Best methods: breath test or stool antigen. Endoscopy only if needed for other reasons.
Once confirmed gone, no need for endless re-tests unless symptoms return.
This step catches failures early so salvage options can be used before resistance gets worse.
What’s Changed and Where Things Stand in 2026
The German S2k guideline (last major update around 2016/2017) still guides much of practice, emphasizing targeted testing and weighing resistance risks.
Globally, newer international reports (like Maastricht VI/Florence from 2022) push harder toward treating all infected people as a way to prevent cancer, favor bismuth quadruple as first-line in high-resistance areas, and stress susceptibility testing where possible.
In Germany, things stay more conservative – no blanket test-and-treat, triple therapy still holds as first option in low-risk cases – but doctors increasingly consider resistance patterns and may lean toward bismuth-based approaches sooner.
Rising resistance worldwide keeps pushing for smarter, tailored regimens over one-size-fits-all.
Bottom Line – Knowledge Is the Best Protection
H. pylori isn’t something to panic about if you have no symptoms. But if you have ulcers, bleeding risks on painkillers, or stubborn indigestion, getting checked can make a real difference.
Treatment works well when done right, heals ulcers, prevents complications, and gives peace of mind. The key is matching the right test and therapy to your situation while keeping an eye on resistance trends.
If stomach issues keep bothering you, talk to your doctor. Simple tests and a short course of meds often solve problems that have dragged on for years.
Have you ever been tested for H. pylori or treated it? What was your experience like? Share below – real stories help everyone understand how this plays out in everyday life.